Medication & Memory: Isn’t there a machine for this?
Gary Wolf
October 12, 2007
In a hospital or a doctor’s office, you are usually asked what medications you have taken recently. Under conditions of distraction, I’m sometimes uncertain if I’ve given a correct answer. I think to myself: “okay, if I’m a professional question-asker, and I’m doubting my memory in this situation, how often are incorrect responses given by people who have more prescriptions and less practice?
We now know the answer.
A study by Dr. Stephen Persell at Northwestern University looked at 119 low income patients, average age 55, under treatment for high blood pressure. Nearly fifty percent were unable to name a single medication listed on their chart. The paper will be published in the November issue of the Journal of General Internal Medicine. (Press announcement here.)

Obviously, there should be a machine to remember this for us. But this is more easily said than done. Even when drugs are administered in a hospital setting, errors are common.
The solution hospitals many beginning to use is to track all drug dispensing with bar codes. It’s a complicated, expensive method, but a paper published in the Archive of Internal Medicine last April reported that the money saved through reduction in “adverse drug events” from implementing bar codes would recoup the investment within one year.

The question now: how can quality-of-care innovations like pharmacy bar codes give us better ability to know and control our own medical information?
Why not give patients a small booklet, similar to the booklet the Savings & Loan banks gave to depositors. Thought these booklets were cheap to produce, their design and the way they were used suggested they were valuable. Customers would hand their booklet to the teller, who would fill in the deposit or withdrawal amount and the new balance.
I’m not suggesting that prescription records be kept only in little paper booklets. No – the booklet would be a patient interface to the electronic prescription records that doctors, hospitals, and pharmacies are beginning to put into a standard electronic form. At the end of a visit to the doctor, we hand our booklet to the receptionist. The receptionist prints out sticky labels and presses them into the booklet – one label per prescription, one page per visit. The label would show the drug name, dosage, and bar code. We could take this booklet with us to the pharmacy. If a generic was substituted, the pharmacist could print out a label and add it to the page.
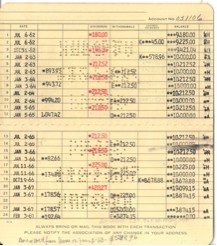

This is not as elaborate as it sounds. The booklet would sit on top of bar code technology that is already being installed. It is just a matter of giving the information to the patient in a handy form: portable, well-organized, and standard. It would work for people of all ages and temperaments, not just for those who like to track their medications online. Because the prescription book is just an interface, it doesn’t matter too much if it gets lost. A new one can be easily made. But it would also function in situations where the online information was not available – for instance, a patient could read it to a nurse over the phone.
This may be wrong and I’d be happy to hear about why.