Talking Data With Your Doc : The Patient
Ernesto Ramirez
March 29, 2012
Data.
Health.
Communication.
In our daily lives, we are keenly aware of the power of each of these individual concepts. However taken together, their influence on our wellbeing, to borrow a phrase from my friend Karen Herzog, “our wholeness”, is exponentially influential. So why do they seem to rarely coalesce during our conversations, discussions, and interactions with the individuals and institutions tasked with tracking, diagnosing, and treating the cracks and fissures in our wholeness?
This is the first in a three-part series about the data we produce about our health and how we communicate that information to the medical system, specifically the providers of care. We’re starting from the perspective of the patient because we’ve all been there. Whether it was a routine check up or a 3AM visit to the emergency room, we’ve all had to relay information to a medical provider about out health. So what happens when we’ve collected, stored, and tried to understand our own health information in preparation for those visits?
Our guide today for the patient perspective of health data communication is Katie McCurdy. Katie is a user experience designer and researcher living and working in New York. She is also living with Myasthenia gravis, an autoimmune disease that causes muscle weakness in voluntary muscles. Like many individuals with autoimmune diseases, Katie spend a lot of time communicating and working with the medical system. These visits, although regular, were a point of contention between Katieand the individuals entrusted with her care. So when she was going to see a new physician for the first time she decided to apply her interaction design knowledge and skill. She’s talked about this on her blog and on the e-patients.net blog so I’ll let here words speak for themselves:
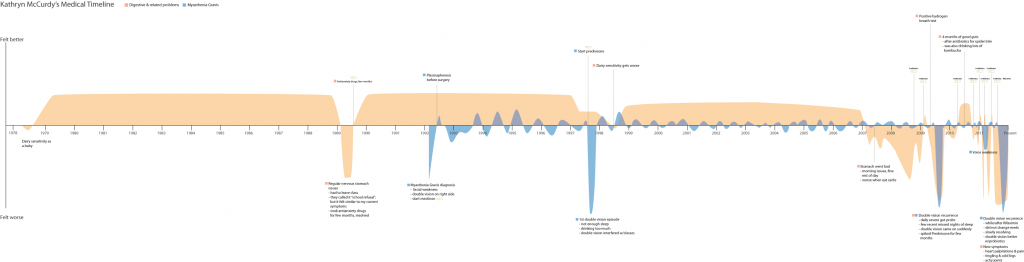
As I was getting ready to see a new doctor, I realized that the best way to tell my story would be to create a medical “life story” timeline that reflected:
- The course of my autoimmune disease
- Severity of my gastrointestinal problems
- Key moments in time when I started and stopped certain medications or took antibiotics
- Any significant dietary changes
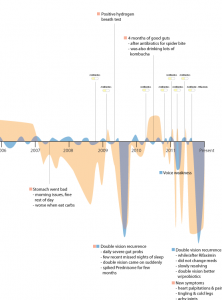
I sketched out the two timelines (autoimmune and gastrointestinal) separately, and then created them electronically using Adobe Illustrator. (I’m an interaction designer by day, so fortunately I had the skills/know-how to create a somewhat legible artifact.) I used a peach color to represent gastrointestinal wellness/symptoms, and a blue color for Myasthenia Gravis.
 Katie was kind enough to answer a few questions and we’re grateful to be able to share her responses here with you today.
Katie was kind enough to answer a few questions and we’re grateful to be able to share her responses here with you today.
QS: Why visualize? Do you think doctors are more receptive to the visual translation of data rather than the raw numbers that are commonly associated with health data?
KM: For me it’s about creating a representation of my history and my health that can be communicated most efficiently. I believe in the power of visualization to help tell stories that wouldn’t be possible with raw data alone. Knowing I would be ‘on the spot’ during my doctor visit put the pressure on to make something that would help me tell my story as succinctly as possible. Also…because I was not tracking my data (it’s all from memory) I didn’t have the raw data to share anyway!
QS: I’ve been thinking about the doc-patient relationship a lot lately. It seems the walls of authority are crumbling as we speak and we’re moving from a “You do this” or “You listen to me” type of authoritative approach to medicine to more conversational. How do you see data and visualizations helping to start and possibly support those conversations.
KM: I see it as, like you said, changing the dynamics of the relationship so that the patient is more of a partner in care. By tracking data, the patient can provide a more refined and nuanced picture of what is really going on with them. By visualizing that data, the patient is helping the doctor absorb the information more painlessly. The patient is providing contextual information about his or her OWN situation that compliments the doctor’s past experience, expertise, and test results.
QS: You mention in your post that the reception from patients and caregivers has been really positive, how would do we help make it a positive and rewarding experience for the providers as well?
KM: I think that giving patients tools to create simple, clean, and attractive visualizations could help make the experience better for doctors. If doctors are presented with high-quality visualizations that tell a coherent story, it may make office visits more efficient. Imagine if the doctor could work with the patient and suggest a type of graph or visualization that would be most helpful.
QS: What tips or advice would you give to someone who is taking their data to their doc for the first time?
KM: I suggest using the data as a storytelling tool. Bring a printed artifact or something on a tablet to refer to, and point out the highlights as you talk about what’s been going on with you. Don’t be disappointed if they don’t comment on your beautiful data and all of the work you put into it. Ask if there is anything you can do to to make the data more legible/easy to understand for the doc.
QS: You mention that self-tracking has given you better insights into your own health and that you’re even trying some self-experimentation like a no-carb diet. How do you think self-tracking and data communication with physicians can support patient-initiated health experimentation?
KM: Ah, I think self-tracking and visualization can help increase patient compliance! My low-carb diet was actually prescribed by my doctor. When I saw on the timeline that my diet changes were strongly correlated with my gastro symptoms improving, it was very reinforcing of my diet behavior. I mentioned antibiotics in my post. Now, if I even think of asking for antibiotics, all I can see in my mind is the number of antibiotics I took as my stomach issues got worse and worse. That is a big change in my outlook that resulted from internalizing the data I was seeing on the timeline.
QS: Who are your design/data viz heros? Anyone who really inspires you in your health visualizations?
KM: I have a few data viz heros! Jer Thorpe, of the new york times, makes beautiful interactive data visualizations and is one of the best speakers I have ever seen. Nicholas Felton, of Feltron and now a designer at Facebook, is a compulsive self-tracker who releases a gorgeous printed yearly report. I love Mortiz Stefaner’s work as well. I am really inspired by the natural world and the work of 19th century plant and wildlife documentor Ernst Haekel. I am also inspired by the awesome patients I’ve met and the folks on e-patients.net who remind me that patients need to be their own advocates.
We also have some questions from Susannah Fox, who was kind enough contribute her thoughts and insights to this piece:
SF: Would Katie care to comment on that from her own experience? That is, is it only recently that she has both found the right tools and that her own clinicians are interested? Had she attempted something earlier, with pencil & paper? What has made the difference?
KM: I never did anything before this apart from bringing notes to my doctor visits – things to remember to say. I literally had a realization one day at work and wrote an email to my personal account with the subject: ‘very important idea.’ 🙂 I think the idea had to incubate for a few years before it bubbled up.last fall.
My goal is to keep pursuing this idea and work toward creating a tool for patients so they can at least assemble their own health timeline, and perhaps even track their data more regularly. I am holding interviews with patients, patient caregivers (or parents), and people who are active self-trackers; if you are interested in donating about 30 minutes of your time, email me at kathryn.mccurdy at gmail.com.
Again, this is part one in a three-part series on the data centric conversation we engage in with the medical community. Look for our next part with insights from Dr. Eric Topol and Dr. Larry Chu next Thursday. If you have questions of comments feel free to discuss on Facebook, Twitter, and here in our comments.